Inside an epidemic
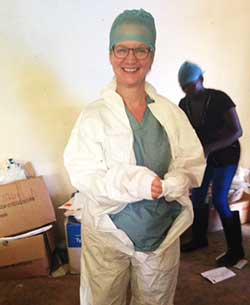
Belinda Fish, MSN ’14, dons protective gear before entering an Ebola treatment unit in Sierra Leone. (Image courtesy of Fish.)
Belinda Fish, MSN ’14, worked her way through the makeshift Ebola treatment unit, sweating in the oppressive African heat. Clad in protective gear and wearing three pairs of gloves, she slid in her rubber boots as she moved from bed to bed. The double-threat of heat exhaustion and dehydration clung to her like the fog that clouded her face shield.
Despite her discomfort, she was determined to deliver the tender care she considers standard: rubbing one patient’s feet, stroking another’s back.
“The patients are scared and they feel terrible. They’re looking at you like you’re a monster, but they’ve gotten used to it for the most part,” says Fish, a chronic care nurse who recently completed a six-week stint with Partners In Health (PIH) in West Africa’s Republic of Sierra Leone.
“I always made sure the patient knew I was there to help them, and that I was sorry for their suffering. The nationals would help with the language barrier, and I’d say, ‘I’m sorry I’m in this nasty outfit. I can’t wait till we see each other in our regular clothes.’”
Paying it forward
In January Fish took an unpaid leave of absence from her work at the University of Michigan Health System’s Chelsea Health Center to volunteer with PIH. She returned stateside in early March and recently completed the “forced vacation” of her 21-day quarantine in compliance with the Centers for Disease Control guidelines administered by the Washtenaw County Health Department. (Conditions of quarantine vary, based on one’s level of risk of exposure to the Ebola virus.)
And though she had volunteered in Kenya, Haiti, and Honduras in the past, Fish had never experienced anything like the Ebola crisis. By traveling to Sierra Leone she was able to fulfill her own mission as a humanitarian – and take away practical lessons about global response and direct patient care under the most extreme resource constraints.
She hopes to share this experience and knowledge as a nursing professor one day, creating a curriculum for nurses here and abroad to better deliver quality public health in resource-poor conditions.
“I couldn’t pass up the opportunity to engage with such a huge public health problem,” says Fish. “I knew that to be on the ground and see how this works was going to be incomparable, professionally and personally.”
Beyond belief
Despite the extensive preparation and training PIH provided, Fish was stunned by the primitive conditions on the ground. Triage centers and treatment units (ETUs) were crude open-air units with tin or grass roofs, surrounded by plastic fencing.
Health care workers mixed their own medications. Buckets of chlorine lined the floor. Thin cloths served as minimal bed linens. Lizards, ants, and other insects were everywhere.
“I knew I was going to see some awful stuff,” Fish says. “[Sierra Leone] has some of the worst health outcomes in the world. And yes, you do some crying. But most of the time you are so intent on just giving the best possible nursing care you can.”
Health care staff entering the ETUs worked in teams — at minimum, two clinicians and a “sprayer” who carried a tank of chlorine to disinfect patient areas. Direct contact with patients was restricted to shifts that maxed out at two hours. After that, conditions became dangerous for staff.
“The limitations on the care are defined by the tolerance and safety of the workers,” Fish says. “It is impossible to make a fabric that is breathable but also impermeable to germs. So basically you are hot, hot, hot. You come out and your scrubs are soaked. You take off your big rubber boots and just pour them out. I have never sweated like that in my life.”
On the home front
Fish was encouraged to hear that during her time in Sierra Leone, a multidisciplinary charette of U-M students, faculty, and staff from the Stamps School of Art & Design, the School of Nursing, the School of Public Health, and the College of Engineering, convened to brainstorm new types of protective gear. Teams designed and executed innovative prototypes, keeping in mind occupational hazards and usability. Fish sees ways those lessons can be applied to many nursing scenarios, including administration of chemotherapy.
“That’s one of the terrific things research institutions like Michigan can do well,” says Fish. “We have brilliant designers, engineers, and so much expertise here. Focusing on the health care workers’ safety is paramount. One of the greatest tragedies of this [Ebola] crisis is how many health care workers died at the onset. They jumped in because they had to.”
Prescription for success
Fish was inspired by the collaboration she saw among global public health care agencies, nongovernmental organizations, and the Ministry of Health in Sierra Leone. Their work transcended the immediate crisis.
“It was great to see the organizations come together to fight this disease and also transform the health system, which really needs support,” she says. “I’m so grateful to have seen that happening in real time.”
Informal connections were just as valuable. Fish and about 70 health care workers lived in a tent city constructed by the Danish army. They enjoyed camp-style meals together, and gathered around a large satellite TV in the evenings to decompress, provide mutual support, and share lessons and best practices from the day.
Though Fish was fortunate to receive a stipend from PIH (which helped offset the financial loss during her unpaid leave), she met three nurses in her cohort of 15 who were not so lucky. Those nurses’ employers did not even offer unpaid leave for the volunteer mission, so the nurses quit their jobs altogether. Health care organizations have a huge opportunity to develop systems that encourage and support volunteerism when public health crises strike, Fish says, because the benefits are far-reaching.
“This land has now seen the response of their global neighbors saying, ‘We want this disease to go away for you. We want you to get better at taking care of yourselves. We’ll partner with you. But we’re not going to take over.’
“We [in the U.S.] have so many resources, and so many people have so little — not just because of poverty, but also because of long-term system failure and injustice. We have to do some work to create justice again.”
Building bridges
As part of her work in Sierra Leone, Fish also supported a number of PIH-funded public health units that had reduced service or shut down during the height of the Ebola crisis. As staff prepared to once again provide the basics of primary health care to local residents, she was able to contribute and learn. She also provided nursing care at the local government hospital.
Fish is now preparing to return to her own patients in Chelsea, and says she feels tremendous gratitude for the moments of joy amid the heartache she witnessed in Sierra Leone. She landed in the country after the Ebola crisis appeared to have peaked, and twice she participated in the closing and burning of triage/holding centers that once catered to patient overflow. Alongside local staff, she spent hours dismantling and hauling torn-down fencing. Then she celebrated with the workers who rejoiced amid the flames.
“What a great symbol of being on the winning side of this crisis,” she says.
And then there’s the 15-year-old girl Fish befriended. The one who beat the odds. Upon her recovery, the girl did get to see Fish in her “regular clothes,” as the nurse once promised. As she prepared to leave the facility for good, the staff gathered for their favorite ritual: tying a new ribbon on the “Survivors’ Tree.”
“It’s a very cool, celebratory thing,” Fish says. “That’s the wonderful part of it.”
(Top image: Fish gathers wood for burning a treatment center that is no longer necessary. Image courtesy of Fish.)






Mark Davis-Craig - 1984
Thank you, Belinda!
Reply
Jen Bellot - 2000, 2002
Belinda, you make nursing proud! Thank you for your sacrifices.
Reply
Ramona Bashshur - 1984
i’m really just blown away by this.
Reply
Amy Spooner - 1995
Great story, incredible woman. Thank you!
Reply