Ice therapy
Muscle sprains, strains, inflammation, and soft tissue trauma or contusion (muscle bruises with ruptured blood capillaries) are relatively common among athletes, industrial workers, and weekend warriors. (You know who you are.) Typical muscle injuries occur when a sudden, strong, compressive force applies to a muscle or when a muscle overworks and fatigues following overload exercise (also known as EIMD — exercise-induced muscle damage).
Clinically, muscle-related injuries usually manifest with localized pain, swelling, reduced range of motion, and tenderness. These damages occur at the molecular level, resulting in transient trauma to individual muscle fibers (myofibrils). This includes necrosis (cell death due to disease, injury, or blood supply failure) and inflammatory cell infiltration — primarily cytokines. Cytokines include a number of substances such as interferon, interleukin, and growth factors secreted by immune cells. Any one or all of these substances are thought to be involved in the pathological pain sensation when muscle(s) become injured.
Muscle healing/repair begins soon after an injury occurs. A tightly synchronized process activates cellular and molecular responses consisting of two interdependent phases, degeneration and regeneration. The repair process appears to be affected by the degree of damage and the interactions between the muscle and the infiltrating inflammatory cells.
Individual muscle fiber regeneration and repair requires a balance between pro-inflammatory and anti-inflammatory factors that determine whether the damage resolves with muscle fiber replacement and reconstitution of a functional contractile apparatus, or with scar formation that may permanently affect function.
Angiogenesis (new blood-vessel formation) and improved vascularization represent key processes in successful muscle regeneration; the processes depend on vascular network restoration for required oxygen and nutrient exchange, and mature muscle-fiber formation.
A long history

Ice application as the preferred treatment of primary and secondary muscle damage and ensuing inflammatory response can be traced as far back as ancient Greece. (Image: iStock.)
Cold therapy (cryotherapy) generally has been accepted as the “universal” therapeutic modality to relieve pain (analgesia). Ice application is now ubiquitous and ingrained as part of the acute injury management process. New research, however, suggests that it may not be the optimal treatment. It may, in fact, act as a hindrance to recovery.
We can trace ice application as the preferred treatment of primary and secondary muscle damage and ensuing inflammatory response to ancient Greece. Hippocrates suggested water therapy could “allay lassitude” in reducing the depletion of energy or strength after injury. His use of ice and snow to treat edema (swelling) has inspired some to credit Hippocrates as “the grandfather of cryotherapy.”
Over time, the way in which cold temperature has been applied to the human body has remained largely unchanged. The most common preferred muscle-injury management procedure involves the RICE method – using rest, ice, compression, and elevation. This initial guideline became deeply rooted in therapeutic applications without any sound scientific evidence.
Modifications of the RICE guidelines changed as research became available, such that RICE morphed into PRICE when “protection” was included in the protocol, (protection, rest, ice, compression, and elevation). Subsequent research suggested that following injury, optimal muscle loading would further enhance recovery so that PRICE was replaced with POLICE (protection, optimal loading, ice, compression, and elevation). The latest and most comprehensive acronym, PEACE & LOVE (protection, elevation, avoid anti-inflammatory drugs, compression, and education & load, optimism, vascularization, and exercise) eliminated the use of ice altogether.
Treating muscle injuries
Icing appears to reduce swelling and inflammation, but how this impacts long-term healing remains controversial and largely undocumented. The number of controlled randomized trials testing the efficacy of any of these protocols remains low, but it should be acknowledged that anything that reduces inflammation also delays healing since the process of inflammation is an essential aspect of recovery itself.Research shows that while cold therapy typically slows soft tissue swelling (edema) and inflammation, it does not hasten the recovery process. This is important since too much or prolonged swelling, which is typically seen in severe joint sprains, has been proved to impede long-term healing. However, when the edema level is not severe, cold therapy may act as a barrier to recovery. When a muscle injury occurs, the body sends signals to the inflammatory cells (macrophages) to release the hormone insulin-like growth factor (IGF-1). These factors initiate healing by killing damaged tissue. However, when ice is topically applied, the cold acts to constrict and impede the transport of inflammatory chemicals to the injured site — and therefore delays the start of muscle healing and recovery.
Conclusions
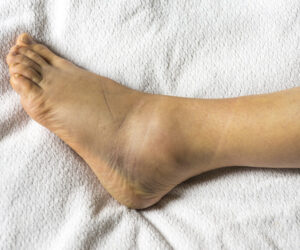
The most common preferred muscle-injury management procedure involves the RICE method – using rest, ice, compression, and elevation. This initial guideline became deeply rooted in therapeutic applications without any sound scientific evidence, Katch says. (Image: iStock.)
The idea of wrapping an injured muscle tightly with ice to accelerate recovery by stopping swelling and moving “waste” from the muscle site is not supported by the evidence. Most research on animals and humans suggests the body is able to adequately remove any fluid accumulation from damaged muscle via movement of lymph through muscle, stimulated by muscle action. Therefore, an extended period of rest following an injury to a tendon, ligament, or muscle is not the best way to accelerate tissue regeneration. Instead, if possible, muscle movement following an injury enhances circulation and subsequent recovery.
Research evidence suggests that the application of ice is only necessary for a short period of time (±2 hr) if swelling and pain reduction is the desired outcome. In many well-controlled studies, longer-term ice use has been found to delay long-term recovery, and possibly damage muscle.
For most people who experience a muscle-related injury that does not require an emergency room visit, rehabilitation should prioritize pain-free movement through a full range of motion as early as possible and gradually progress to higher intensities and more complex movements.
References
- Bleakley, C., et al., “The use of ice in the treatment of acute soft-tissue injury: A systematic review of randomized controlled trials.” The American Journal of Sports Medicine 2004;32(1):251.
- Bleakley C., et al., “Cryotherapy for acute ankle sprains: A randomized controlled study for two different icing protocols.” British Journal of Sports Medicine. 2006;40(8),700.
- Bleakley, C.M., et al., “PRICE needs updating, should we call the POLICE?” British Journal of Medicine. 2012;46: 220.
- Canale, S.T., “A chronicle of injuries of an American intercollegiate football team.” The American Journal of Sports Medicine. 1981;9,384.
- Ciolek, J.J., “Cryotherapy. Review of physiological effects and clinical application.” Cleveland Clinic. 1985;52:193.
- Crystal, N.J, et al., “Effect of cryotherapy on muscle recovery and inflammation following a bout of damaging exercise.” European Journal of Applied Physiology. 2013;113: 2577.
- Cullen, M.L., et al., “Passive recovery strategies after exercise: A narrative literature review of the current evidence.” Current Sports Medicine Reports. 2021;20(7):351.
- Doherty, C., et al., “Treatment and prevention of acute and recurrent ankle sprain: An overview of systematic reviews with meta-analysis.” British Journal of Medicine. 2017;51: 113.
- Dubois, B., Esculier, J.F., “Soft-tissue injuries simply need PEACE and LOVE.” British Journal of Medicine. 2020;54: 72.
- Grant, A.E., “Massage with ice (cryokinetics) in the treatment of painful conditions of the musculoskeletal system.” The Archives of Physical Medicine. 1964;45:233.
- MacAuley, D.C., “Ice therapy: How good is the evidence?” International Journal of Sports Medicine. 2001;22: 379.
- Miranda, J.P., et al., “Effectiveness of cryotherapy on pain intensity, swelling, range of motion, function, and recurrence in acute ankle sprain: A systematic review of randomized controlled trials.” Physical Therapy in Sport. 2021;49:243.
- Mirkin, G., Hoffman, M., “The Sports Medicine Book.” Boston: Little, Brown and Company, 1978.
- Palmieri, R.M., et al., “Arthrogenic muscle response to a simulated ankle joint effusion.” British Journal of Medicine. 2004;38: 26.
- Tipton, M.J., et al., “Cold water immersion: Kill or cure?” Experimental Physiology. 2017;102(11):1335.
- Tittley, J., et al. “Should ice application be replaced with neurocryostimulation for the treatment of acute lateral ankle sprains?” Journal of Foot and Ankle Research. 2020;13:69.
- Tseng, C.Y., et al., “Topical cooling (icing) delays recovery from eccentric exercise-induced muscle damage.” The Journal of Strength and Conditioning Research. 2013;27:1354.
- van den Bekerom, M.P., et al., “What is the evidence for rest, ice, compression, and elevation therapy in the treatment of ankle sprains in adults?” Journal of Athletic Training. 2012;47:435.
- Vuurberg, G., et al., “Diagnosis, treatment, and prevention of ankle sprains: Update of an evidence-based clinical guideline.” British Journal of Medicine. 2018;52:956.
- Wang, Z.R., Ni, G.X., “Is it time to put traditional cold therapy in rehabilitation of soft-tissue injuries out to pasture?” World Journal of Clinical Cases. 2021;16;9(17):4116-4122.
- West, J.B., “Galen and the beginnings of Western physiology.” The American Journal of Physiology-Lung Cellular and Molecular Physiology. 2014;307(2):L121–L128.





D Hatcher - 1973, 1983
The key is that we are homeothermic animals, so repeated icing immediately after an injury (for the first couple post injury hours — 20 minutes in, 25 minutes out to warming) pulses fresh blood to the area as it warms after icing and flushes waste away as it cools with icing. The temporary alleviation of pain can also aid muscle movement during the warming period.
Reply
Frank Velasquez - 1993
Working as an ATC, CSCS at both professional and amateur levels for the past 30 years I have always been an advocate for applying ice to acute strains and sprains resulting in positive outcomes. There are better options with today’s medical technology / modalities that not everyone has access to use… just about everyone has access to cold therapy… I do agree in holding off on NSAID consumption as well as using and loading the injured body part ASAP to accelerate healing. Great work as always Dr Katch! It’s been a while… have always remembered my time spent in your classrooms… best wishes and Go Blue! FV
Reply