First in the world
Kaiba Gionfriddo was just a newborn when he turned blue because his little lungs weren’t getting the oxygen they needed. Garrett Peterson spent the first year of his life in hospital beds tethered to a ventilator, being fed through his veins because his body was too sick to absorb food. Ian Orbich’s heart stopped before he was even six months old.
Three babies all had the same life-threatening condition: a terminal form of tracheobronchomalacia, which causes the windpipe to periodically collapse and prevents normal breathing. There was no cure and life-expectancies were grim.
The three boys became the first in the world to benefit from groundbreaking 3D-printed devices that helped keep their airways open, restored their breathing, and saved their lives at the University of Michigan’s C.S. Mott Children’s Hospital. Researchers have closely followed their cases to see how well the bioresorbable splints implanted in all three patients have worked, publishing the promising results in a recent issue of Science Translational Medicine.
Looking good
“These cases broke new ground for us because we were able to use 3D printing to design a device that successfully restored patients’ breathing through a procedure that had never been done before,” says senior author Glenn Green, MD, associate professor of pediatric otolaryngology at C.S. Mott Children’s Hospital.
“Before this procedure, babies with severe tracheobronchomalacia had little chance of surviving. Today, our first patient, Kaiba, is an active, healthy 3-year-old in preschool with a bright future.“The device worked better than we could have ever imagined,” he continues. “We have been able to successfully replicate this procedure and have been watching patients closely to see whether the device is doing what it was intended to do. We found this treatment continues to prove to be a promising option for children facing this life-threatening condition that has no cure.”
The published findings suggest that early treatment of tracheobronchomalacia may prevent complications of conventional treatment such as a tracheostomy, prolonged hospitalization, mechanical ventilation, cardiac and respiratory arrest, food malabsorption, and discomfort. None of the devices, which were implanted in then 3-month-old Kaiba, 5-month-old Ian, and 16-month-old Garrett, have caused any complications.
More good news
The findings also show that the patients were able to come off of ventilators and no longer needed paralytics, narcotics, and sedation. Researchers noted improvements in multiple organ systems. Patients were relieved of immunodeficiency-causing proteins that prevented them from absorbing food so that they no longer needed intravenous therapy.
Green worked with U-M colleague Scott Hollister, PhD, professor of biomedical engineering and mechanical engineering, and associate professor of surgery. Using 3D printing they created and implanted customized tracheal splints for each of the young patients. The device was created directly from CT scans of each individual trachea, integrating an image-based computer model with laser-based 3D printing.
The specially designed splints were sewn around the children’s airways to expand the trachea and bronchus and give it a skeleton to aid proper growth. Experts tracked the growth with CT and MRI scans. The device was shown to open up to allow airway growth for all three patients, and the material will be reabsorbed by the body over time.
Clear!
Doctors received emergency clearance from the FDA to do the procedures.
“We were pleased to find that all of our cases so far have proven to improve these patients’ lives,” Green says. “The potential of 3D-printed medical devices to improve outcomes for patients is clear, but we need more data to implement this procedure in medical practice.”
Authors say the recent report was not designed for device safety and that rare potential complications of the therapy may not yet be evident. However, Richard G. Ohye, MD, head of pediatric cardiovascular surgery at C.S. Mott who performed the surgeries, says the cases provide the groundwork to potentially explore a clinical trial that could help other children with less-severe forms of tracheobronchomalacia in the future.
Progress report
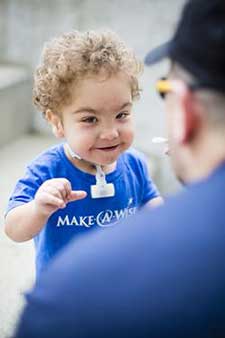
Kaiba is now a curious, active 3-year-old who loves playing with his siblings. He recently saw his favorite character Mickey Mouse at Disney World thanks to the Make-a-Wish Foundation. Last month he was back at Mott for a follow-up appointment.
The splint is dissolving just how it’s supposed to and doctors expect that eventually, Kaiba’s trachea will reflect that of his peers with no signs of the tracheobronchomalacia that nearly killed him as a newborn.
“The first time he was hospitalized, doctors told us he may not make it out,” his mother, April Gionfriddo, remembers. “It was scary knowing he was the first child to ever have this procedure, but it was our only choice and it saved his life.”
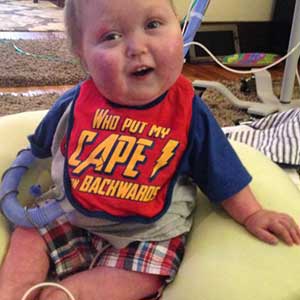
Now an energetic 2-and-a-half-year-old with a contagious laugh, Garrett is able to breathe on his own and spend his days ventilator-free. Ian is now 17 months old, and is known for his huge grins, enthusiastic high fives, and love for playing with his big brother, Owen. Ian had the splint procedure done at Mott one year ago.
“We were honestly terrified, just hoping that we were making the right decision,” his mother, Meghan Orbich, remembers. “I am thankful every single day that this splint was developed. It has meant our son’s life. I am certain that if we hadn’t had the opportunity to bring Ian to Mott, he would not be here with us today.”
This story was reprinted courtesy of the University of Michigan Health System.
- Support this important research by making a gift to the 3D-Printed Airway Splint Fund.
- Watch a video demonstrating 3D printing
- Read blog post from Dr. Glenn Green that goes behind the scenes on what led to the 3D printed devices to restore breathing in babies with tracheobronchomalacia.
- See more on Kaiba’s story
- See more on Garrett’s story
Additional Authors: Robert J. Morrison, Scott J. Hollister, Matthew F. Niedner, Maryam Ghadimi Mahani, and Richard G. Ohye, all of U-M. Albert H. Park, of University of Utah; Deepak K. Mehta, of the Children’s Hospital of Pittsburgh of University of Pittsburgh Medical Center.
Funding: This work was funded in part by the National Institutes of Health (grant R21 HD076370-01) Morrison is supported by NIH grant T32 DC005356-12.
Disclosure: Hollister and Green have filed a patent application related to the device.
Reference: “Mitigation of Tracheobronchomalacia with 3D-Printed Personalized Medical Devices in Pediatric Patients,” Science Translational Medicine, April 29, 2015.





John Korstad - 1980 (PhD)
Thank you for your encouraging and uplifting story. I’m very proud of the UM researchers, support staff, parents, and especially the beautiful children who are alive today because of this innovative research! 🙂
Reply