What is gluten?
 The availability of gluten-free products in the marketplace has jumped 25 percent in the last five to seven years. Most people purchase gluten-free products under the assumption that eliminating gluten from their diet is good for their health, whether or not they have been diagnosed with a gluten sensitivity.
The availability of gluten-free products in the marketplace has jumped 25 percent in the last five to seven years. Most people purchase gluten-free products under the assumption that eliminating gluten from their diet is good for their health, whether or not they have been diagnosed with a gluten sensitivity.
Gluten is safe for everyone, except those who have some variant of irritable bowel syndrome (IBS). Several conditions are listed under the IBS “umbrella.” These include celiac disease, gluten allergy or sensitivity, lactose intolerance, specific wheat intolerance syndrome, small intestinal bacterial overgrowth, and short-chain carbohydrate sensitivities. (See “FODMAPs” below.)
Sales of gluten-free products reached $15 billion in 2016, a 50 percent increase over 2013, and there appears no abatement of this exponential increase.
How did we get here?
In 2011, Australian researchers found gluten caused gastrointestinal distress in some individuals without celiac disease – a clinical condition now referred to as nonceliac gluten sensitivity or NCGS.
This double-blinded, randomized, and placebo-controlled experiment was one of the strongest pieces of evidence that NCGS – also called “gluten intolerance,” was a genuine condition. The press highlighted this study, which contributed to the meteoric sales of gluten-free food.
 However, a follow-up experiment by the same researchers produced different results. This time the scientists used more rigor to control other variables that might cause adverse gluten reactions. In this experiment, they controlled or removed all potential dietary triggers for gastrointestinal symptoms, including lactose (from milk products), certain preservatives like benzoates, propionate, sulfites, and nitrites, and fermentable, poorly absorbed short-chain carbohydrates.
However, a follow-up experiment by the same researchers produced different results. This time the scientists used more rigor to control other variables that might cause adverse gluten reactions. In this experiment, they controlled or removed all potential dietary triggers for gastrointestinal symptoms, including lactose (from milk products), certain preservatives like benzoates, propionate, sulfites, and nitrites, and fermentable, poorly absorbed short-chain carbohydrates.
Participants included 37 people who did not have celiac disease, but who said their GI symptoms improved on a gluten-free diet. Subjects ate one of three diets that included either high gluten (16 grams per day), low gluten (2 grams per day) or nongluten (placebo). Each subject shuffled through each diet so they could serve as their own controls, and none knew what specific diet he or she was eating. Results from this experiment revealed that each diet, whether it included gluten or not, prompted subjects to report a worsening of GI symptoms. Reported levels of abdominal pain, bloating, nausea, and gas all increased, even with the placebo, nongluten diet.
These data indicated a nocebo effect – when a negative expectation of a phenomenon causes it to have a more negative effect than it otherwise would. In essence, individuals reported GI distress without any apparent physical cause. The participants expected the diets to make them sick, and they did.
The above findings led the researchers to retract conclusions from their first experiment. They stated, “In contrast to our first study . . . we could find absolutely no specific response to gluten.” Results of this follow-up experiment were not covered in the press, of course.
Why do people choose gluten-free options?
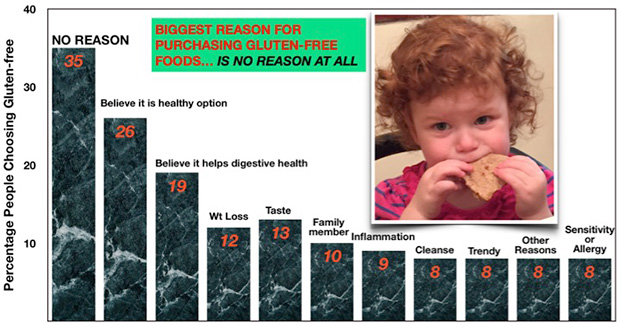
In a 2015 survey, more than 35 percent of all people who purchased gluten-free products said the reason for spending the extra money for these specialized items was . . . “No reason at all!” In fact, in this study only 8 percent or less of people who chose gluten-free products did so because of celiac disease or a verified gluten sensitivity or allergy.
In another study, 86 percent of individuals who reported gluten-related symptoms had neither a gluten allergy or specific sensitivity, or verified celiac disease, or a wheat allergy. The researchers concluded that self-perceived gluten-related symptoms are rarely indicative of the presence of true gluten intolerance.
Why should one avoid gluten?
Celiac Disease
Celiac disease, which affects an estimated 1 in 133 Americans, represents the most severe form of gluten intolerance. First-degree relatives of people with celiac disease – parents, siblings, and children have a one in 10 risk compared to one in 100 in the general population. Celiac disease represents an autoimmune disorder where the body treats gluten protein as a foreign invader and attacks the gluten, as well as the lining of the gut where gluten resides after ingestion. Celiac disease affects men and women of all ages and races. It is estimated that 83 percent of Americans who have celiac disease are undiagnosed or misdiagnosed with other conditions.The most common symptoms of celiac disease are digestive discomfort, bloating, diarrhea, constipation, headache, tiredness, skin rashes, depression, weight loss, and foul-smelling feces. Some people with celiac disease do not have digestive symptoms, but may have other symptoms like tiredness or anemia.
People with undiagnosed celiac disease incur medical costs averaging $4,000 more than healthy individuals. There are no pharmaceutical treatments or cures for celiac disease – a 100 percent gluten-free diet represents the only existing treatment.Non-celiac gluten sensitivity
Many people suffer from symptoms that seem related to gluten, but celiac disease and allergies have been ruled out. These individuals are said to have nonceliac gluten sensitivity. Research estimates 18 million Americans have some form of gluten sensitivity – that’s six times the amount of those with celiac disease.
Irritable bowel syndrome (IBS)
Irritable bowel syndrome (IBS) is a group of symptoms similar to gluten intolerance— including abdominal pain and changes in the pattern of bowel movements but without any evidence of direct underlying small-intestine damage. Common among people with IBS are such afflictions as anxiety, depression, and chronic fatigue syndrome. Whether these are causes or results of IBS is not clear. Nevertheless, studies show many individuals with IBS benefit from trying a gluten-free diet.
FODMAPs
FODMAPs are short-chain carbohydrates found in many foods (including wheat) and are poorly absorbed in the small intestine, in some people. The acronym FODMAP stands for: Fermentable (sugars broken down by bacteria in the large bowel); Oligosaccharides (a sugar polymer containing two to 10 simple sugar molecules); Disaccharides (a double sugar molecule); Monosaccharides (a single sugar molecule); and Polyols (a sugar alcohol).
In susceptible individuals, when FODMAPs are consumed they draw in water and produce carbon dioxide, hydrogen, and/or methane gas that cause the intestine to stretch and expand, often resulting in abdominal pain, bloating, visible abdominal distension, and other symptoms, similar to symptoms to celiac disease.
Common FODMAPs include: fructose (fruit sugars); lactose (dairy sugar in milk); dructans (similar to fructose and found in some vegetables and grains); falactans (found in legumes); and polyols (sugar alcohols like xylitol, sorbitol, maltitol, and mannitol commonly found in artificial sweeteners and chewing gum).
Are you gluten sensitive?
Digestive discomfort to certain foods represents the most common indication of gluten intolerance. Screening for celiac disease involves blood testing to screen for specific antibodies, the most common is the tTG-IgA antibody test. If positive, a tissue biopsy is usually recommended to confirm presence of celiac disease.
With a negative celiac disease diagnosis, the best way to reveal gluten sensitivity is to follow a strict gluten-free diet for a few weeks to monitor symptoms. Then, reintroduce gluten in the diet and again monitor symptoms. If symptoms don’t improve on a gluten-free diet, and don’t get worse with reintroduction of gluten, then the culprit is other than gluten.
Common foods containing gluten:
• Breads
• Crackers
• Seasonings and spice mixes
Gluten-containing foods to avoid with gluten tolerance:
Wheat is one of the main staples of a western diet and is public enemy No. 1 for those with gluten intolerance. In addition to pure wheat, all of its forms also should be avoided. These include:
- Wheat starch
- Wheat bran
- Wheat germ
- Couscous
- Cracked wheat
- Durum
- Einkorn
- Emmer
- Farina
- Faro
- Graham flour
- Kamut
- Matzo
- Semolina
- Spelt
- Fu (common in Asian foods)
- Barley
- Bulgur
- Rye
- Triticale and mir (a cross between wheat and rye)
- Seitan
- Oats (Oats themselves don’t contain gluten, but are often processed in facilities that produce gluten)
Gluten presents in other ingredients as well:
- Barley malt
- Chicken broth
- Seasonings and spice mixes
- Malt vinegar
- Some salad dressings
- Soba noodles
- Some condiments
- Most veggie burgers
- Soy sauce
Foods without gluten:
- Fruits and vegetables
- Beans
- Seeds
- Legumes
- Nuts
- Potatoes
- Eggs
- Dairy products
- Oils and vinegars
- Corn
- Rice
- Fish
- Lean beef
- Chicken
- Seafood
Gluten-free grains and foods:
- Amaranth
- Arrowroot
- Buckwheat
- Cassava
- Millet
- Quinoa
- Rice
- Sorghum
- Soy
- Tapioca
For baking, use these flours:
- Buckwheat
- Corn
- Millet
- Rice
- Sorghum
- Quinoa
- Chickpea
References
- Biesiekierski, J.R., et al. 2013. “Is gluten a cause of gastrointestinal symptoms in people without celiac disease?” Current Allergy Asthma Report; 13(6):631-8.
- Biesiekierski, J.R., et al. 2013. “No effects of gluten in patients with self-reported non-celiac gluten sensitivity after dietary reduction of fermentable, poorly absorbed, short-chain carbohydrates.” Gastroenterology; 145(2):320-8.
- Borghini, R., 2017. “New insights in IBS-like disorders: Pandora’s box has been opened — A review.” Gastroenterology and Hepatology From Bed to Bench; 10(2):79-89.
- Capannolo, A., et al. 2015. “Non-celiac gluten sensitivity among patients perceiving gluten-related symptoms.” Digestion; 92(1):8-13.
- Lundin, K.E., Alaedini, A. 2012. “Non-celiac gluten sensitivity.” Gastrointestinal Endoscopy Clinics of North America; 22(4):723-34.
- Valenti, S., et al. 2017. Gluten-related disorders: certainties, questions and doubts. Annals of Medicine; 11:1-13.
- Varjú, P., et al. 2017. “Low fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAP) diet improves symptoms in adults suffering from irritable bowel syndrome (IBS) compared to standard IBS diet: A meta-analysis of clinical studies.” PLoS One. 2017. Aug. 14;12(8).
- Watkins, R.D., Zawahir, S. 2017. “Celiac disease and nonceliac gluten sensitivity.” Pediatric Clinics of North America; 64(3):563-576.
- “Understanding celiac disease,” www.celiac.org.
- “Percentage of U.S. adults trying to cut down or avoid gluten in their diets reaches new high in 2013,” npd.com.




Muffy MacKenzie - 1985
VERY informative Dr. Katch. My life changed 15 years ago when I cut gluten and diary out of my diet. My many throat and ear infections cleared up and my fatigue diminished. I do not need any more proof then that, but appreciate you spelling this out thoughtfully.
PS the gluten free products out there, though they offer an opportunity for a pasta or piece of toast, etc. do not taste good nor do they seem at all healthy! And they are bloody expensive.
Reply
Mary Niester - 1999
Great article! I wanted to give a shout out to the GI dietitians at U of M. They provide individualized nutrition therapy and counseling and are great at sorting out the mountain of nutrition information out there: http://www.uofmhealth.org/conditions-treatments/digestive-and-liver-health/our-care-team
Reply
Russell Lyons - 1983
Under “Other gluten-containing grains”, this article lists seitan. In fact, seitan is made from wheat; it is vital wheat gluten. If you are sensitive to gluten, you have to avoid seitan, but if not, it is a delicious source of almost pure protein.
Reply
Nancy Mosher - 1969
Wheat bran is listed under “Foods Without Gluten” which is incorrect. This could have serious implications for persons who cannot tolerate gluten. Otherwise this is an informative article.
Reply
Deborah Holdship
Nancy, thank you so much for pointing that out. That regrettable error was made on the editing side (while creating the bulleted tables), not by Dr. Katch.
Reply
Arlene Kufchock - 1992
Thank you for this article. My diet relied on gluten until 4 years ago (yet always contained plenty of healthy vegetables and minimal meat). Now I thrive best when I eliminate gluten (I’m not celiac). Packaged processed gluten free foods often add in other components detrimental to my body. Home cooked whole foods are time consuming, so I joined my nutritionist’s group meetings where we learn, among other things, to prepare a week’s nutritious meals in 2 hours. My friends there, led by our nutritionist, provide the upbeat supportive base for my kitchen pantry transformation to clean, organic, whole food sources. The exchange of ideas at this group is essential to my positive cooking habits. I’ve moved a lot and found the key is meeting up with local nutritionally minded people to exchange clean local food source knowledge.
Reply
Ethel Larsen - 1972
Another helpful article. Thank you again.
Reply
Christopher Lumpkin - 1998
Thanks for this informative and well-written article. Is anyone aware of studies that have been conducted regarding a link between IBS symptoms and back injuries? Several years ago, I suffered an injury in the thoracic spinal region and immediately started experiencing IBS symptoms.
Reply
Beniko Hana - 3
A gluten-free diet is essential for most people with gluten allergies or celiac disease. Because any person with celiac disease will experience abdominal pain when they ingest food containing gluten as their body reacts by damaging the small intestine.
Reply
Buckwheat Pasta - 3
Soba is a very common menu Japanese people regularly eat and is available at various types of eateries, from specialty restaurants to tachigui shop. Depending on the shop, the percentage of buckwheat flour in soba noodles typically ranges between 40% and 100%. In Japan, soba noodles can be found in a variety of settings, from “fast food” places to expensive specialty restaurants.
Reply